Data Exchange Framework Stakeholder Advisory Group Meeting #2
Scenario Development and Data Exchange Issue Identification
Last week, the Data Exchange Framework Stakeholder Advisory Group convened to continue its important work to develop recommendations for the California Health and Human Services (CHHS) Data Exchange Framework (DxF). The DxF will govern the required exchange of health information by 2024 – impacting hospitals, providers, health plans, and Californians across the state. This was the second of nine scheduled meetings; a recap of the inaugural meeting can be found on our website.
The Advisory Group reviewed the proposed roadmap for the development of the DxF “end-product” and focused on the first step: “Scenario Development & Data Exchange Issue Identification”

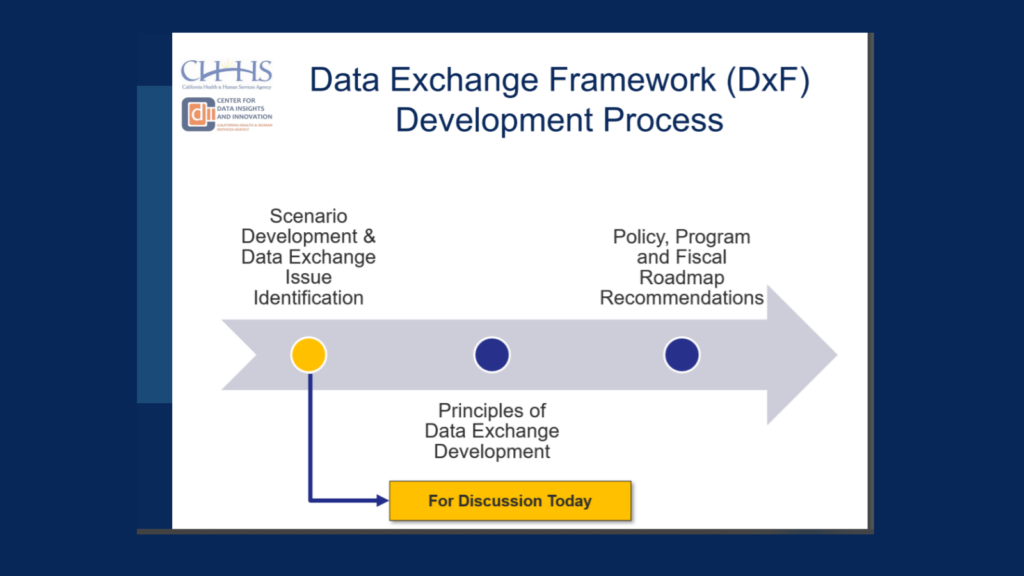
Scenarios are a potential event, combination of events, or set of activities that would require the exchange of health and/or human service information between organizations. A deep dive into each of the six scenarios can be found in the pre-read materials.

There was healthy discussion around each scenario, including missing “Actors” (i.e., organizations required to exchange information to address the individual’s needs) and additional scenarios to consider. Here’s a look at some of the key themes that emerged across multiple scenarios:
- One of the main missing “Actors” in most of the scenarios is the individual patient. Individuals play a critical role in managing their health and the exchange of their health information. This builds on a key theme raised during the first meeting – that the role of the patient in “patient-centered” care should be “front and center.”
“Our charge starts with Californians…so a use case that really looks at a consumer perspective of them being able to have access to all of their data sets seems to me to be worth us giving some thought to.”
“With one exception, the scenarios do not have any information flows with the individual at the center of care. They are actors.”
“It’s crucial that we put consumers at the heart of how we design the data systems. How will consumers access this data, both to update/provide info, and get information that is crucial for managing their health?”
– Amanda McAllister-Wallner, CA LGBTQ Health & Human Services Network Director,
(delegate for Anthony E. Wright), Health Access California
- The “Actors” in these scenarios need to include non-provider sectors such as payers, behavioral health, and social services that play a role in the individual’s health and wellbeing. Members and public commenters agreed that coordination among these groups is essential in addressing social determinants of health and managing population health.
“…Health plans have a key role in CalAIM and thus are a critical actor in both collection and sharing of timely data.”
“There’s an opportunity here, and most vitally in the subcommittees, to bring in some of the administrative policies that can be relaxed…to help this particular area as we talk about behavioral health and SDOH.”
“The WIC program, which serves over about 1 million Californians is a critical support for our pregnant women and our youngest children. It’s also a program that requires medical documentation. To be eligible for services, participants have to provide proof of pregnancy, height and weight measurements, blood work, and medical documentation. Yet there’s no pathway for the exchange of information to the WIC program from medical providers.”
“We need to be thinking about bi-directional [exchange] with the social services of the community-based organizations.”
- Building on the two points above, there was enthusiasm in the Zoom chat among members to add a CalAIM focused scenario specifically around Enhanced Care Management (ECM).
“Would be great to have a scenario around ECM providers and what they need to do to create, manage, update, and share a shared care plan.”
“Support Williams point about creating a platform that will flex to include data from emerging social service technologies and need to include social determinants of health data”
“Right! Shared care plans should be elevated in the scenarios, including the need to establish process/standards for care plans and the sharing of them.”
- For all scenarios, providers and health plans need to be able to aggregate and assemble data from different sources to identify key insights and support population health:
“There’s a cross-cutting infrastructure gap across all these use cases, which is the ability to bring in data from multiple sources, integrate the data using patient matching, clean the data, and make them available for these sources. We need to define data exchange to include data management to make it useful.”
“The community is not only concerned about health data collection but how it’s being used. I’m hoping to see some principles around accountability, consent, oversight, and training of the stakeholders who are accessing data.”
– Lori Hack, Interim Executive Director,
California Association of Health Information Exchanges (CAHIE)
Both on-screen and in the chat, members and public commenters discussed the need to leverage existing exchange and use national standards that are already broadly used.
The meeting closed with an update on the Data Sharing Agreement (DSA) Subcommittee, which will comprise 10 to 15 individuals with technical and legal expertise. The DSA Subcommittee will be appointed by mid-October.
As the state’s largest nonprofit health data network, Manifest MedEx will continue to share updates from the front-line on this important initiative to transform care in our state. This is a critical, bold step towards making health care better for Californians and building the health information network Californians deserve.
We look forward to bringing the voice of our communities and participants to this ground-breaking work as it continues to develop.
The Advisory Group will meet next on November 10, 2021, from 10:00 AM to 12:30 PM. We invite you to follow @ManifestMedEx on Twitter for live tweets, share your thoughts with us at https://www.manifestmedex.org/contact/, and stay tuned for more updates!